A functional medicine provider spends 75 minutes with a new patient reviewing a detailed health history, lab work from three different labs, diet logs, sleep data, and a long list of symptoms that don’t fit neatly into a single diagnosis code. The visit is thorough, clinically meaningful, and exactly what the patient needed.
Then the billing question comes up: How do you bill for that time?
This is one of the most common operational challenges in functional and integrative medicine. Visits are longer. Care is more complex. Communication happens between visits. And the traditional fee-for-service model doesn’t always fit the way these practices actually deliver care.
That’s why billing functional medicine often involves a mix of time-based coding, cash-pay services, memberships, and packages.
But the key word here is mix. And mixing models requires structure.
Why Billing Functional Medicine Is Different
Functional medicine doesn’t follow the typical 10–15 minute visit model. New patient visits often run 60–90 minutes. Follow-ups may be 30–45 minutes. Providers review extensive labs, write detailed care plans, and communicate with patients between visits through portals and messaging.
All of that time matters. But it has to be documented and billed correctly.
Common services in functional medicine that don’t fit neatly into traditional billing models include:
- Long initial visits
- Extensive record review
- Care plan development
- Lab interpretation
- Nutrition and lifestyle counseling
- Supplement protocol management
- Frequent follow-ups
- Portal communication between visits
If clinics try to force all of this into a standard E/M visit without using time-based billing or cash-pay models appropriately, they either lose revenue or create compliance risk.
Understanding Time-Based E/M Coding
For many functional medicine visits, time-based E/M coding is the most appropriate billing method when billing insurance.
Current E/M guidelines allow providers to select office visit levels based on total time spent on the date of the encounter, not just face-to-face time.
This is extremely important for functional medicine providers because so much work happens outside the exam room.
What Counts Toward Time
When billing functional medicine using time, total time may include:
- Reviewing patient records and labs before the visit
- Face-to-face visit time
- Counseling and education
- Documenting in the chart
- Ordering labs, supplements, or medications
- Communicating with the patient on the same day
- Care coordination related to that visit
It does not include time spent on days before or after the visit.
That distinction matters for documentation.
Common Time-Based E/M Codes
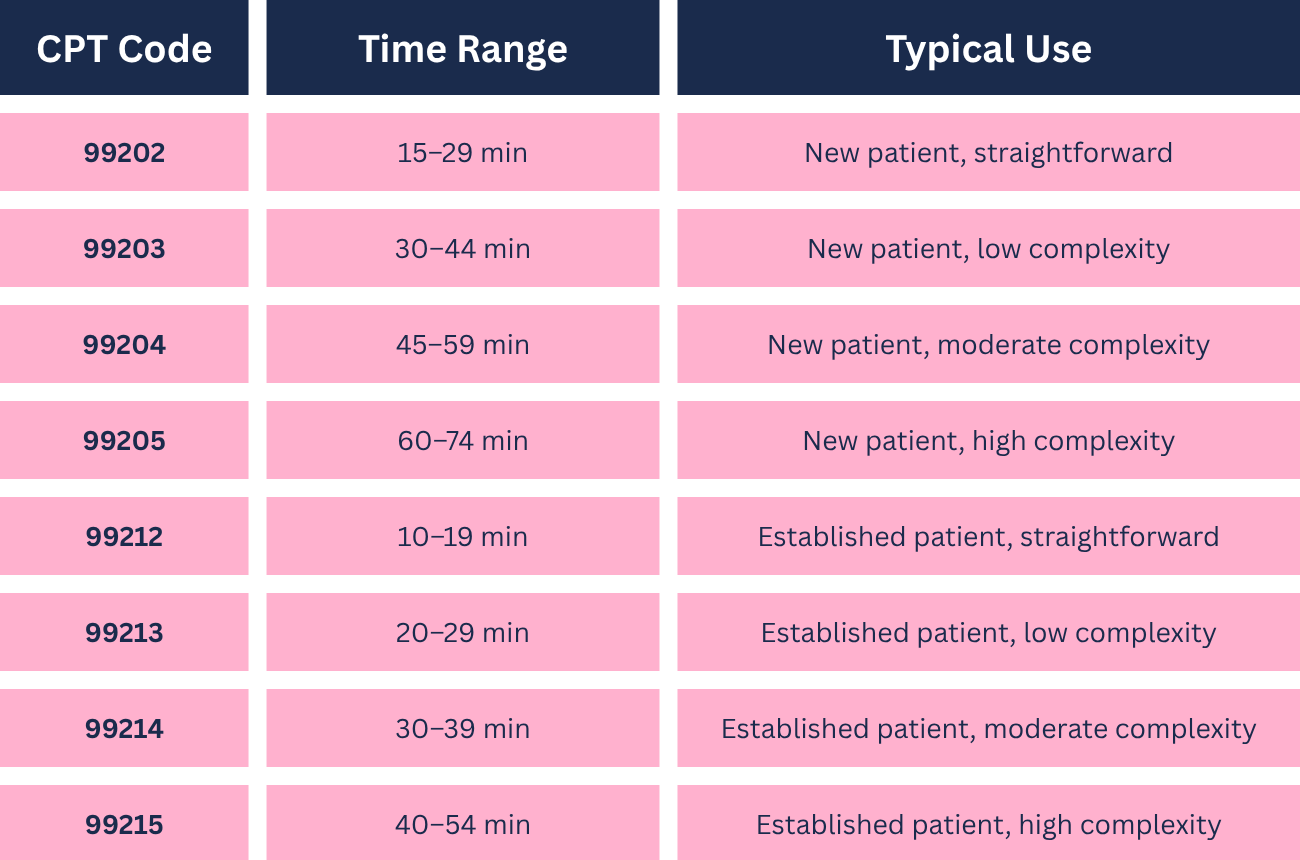
For a deeper breakdown of these codes, explore our CPT® Code Definitions.
Many functional medicine new patient visits may fall into 99205 when time is documented correctly, but the documentation must clearly state total time and what was done.
To learn more about commonly used CPT codes download our guide here.
Documentation Requirements for Time-Based Billing
If you are billing functional medicine visits based on time, your documentation should support that time. This is where many clinics make mistakes.
A compliant time-based note should include:
- Total time spent on the date of the visit
- A summary of what that time included
- Medical necessity for the visit
- Assessment and plan
- Diagnoses
- Patient education and counseling
- Orders and care coordination
Without a time statement, billing functional medicine based on time becomes difficult to defend.
When Cash-Pay Models Make More Sense
Many functional medicine clinics choose cash-pay models because insurance reimbursement often does not reflect the time and complexity involved in this type of care.
Common cash-pay structures include:
Membership Models
Patients pay a monthly fee that may include:
- A certain number of visits per year
- Messaging access
- Lab review
- Care plan updates
- Discounts on supplements or services
Package-Based Care
Examples include:
- 3-month gut health program
- 6-month hormone optimization program
- Weight loss program
- Longevity program
- Detox program
Hybrid Models
Some clinics use a hybrid approach:
- Bill insurance for covered visits using time-based E/M coding
- Charge cash for non-covered services such as:
- Advanced lab interpretation
- Nutrition counseling (if not billable)
- Supplement protocols
- Program fees
- Membership access
- Body composition testing
- Health coaching
Billing functional medicine in a hybrid model requires clear financial policies and very clear documentation so services are not double-billed.
Financial Policies and Compliance Considerations
This is where functional medicine billing can get risky if clinics are not careful.
If you are billing insurance and charging cash, you must clearly separate:
- Covered services
- Non-covered services
- Membership fees
- Program fees
- Supplements and products
- Lab fees
Patients should sign financial policies that explain:
- What is billed to insurance
- What is cash-pay
- What memberships include
- What happens if insurance denies a claim
- Refund policies
- Cancellation policies
From a compliance standpoint, transparency is critical. From a business standpoint, it also prevents a lot of hard front-desk conversations.
Operational Challenges in Billing Functional Medicine
Most functional medicine billing problems are not coding problems. They’re workflow problems.
Common operational issues include:
- Providers forget to document total time
- Staff don’t know whether to bill insurance or charge cash
- Membership benefits are tracked in spreadsheets
- Packages are sold but not tied to visits in the schedule
- Labs are ordered but not linked to a billable visit
- Portal time is not tracked
- Claims are undercoded because time wasn’t documented
- Revenue reporting is unclear because services are split between systems
When billing functional medicine, your scheduling system, EHR, and billing system all need to work together. Otherwise, things fall through the cracks.
Practical Takeaways for Functional Medicine Clinics
If your clinic is working on improving billing functional medicine services, focus on these areas first:
- Train providers on time-based E/M coding.
- Require total time documentation for longer visits.
- Create clear financial policies for cash-pay services.
- Clearly separate insurance-covered vs. non-covered services.
- Track memberships and packages in a system, not a spreadsheet.
- Make sure lab orders are tied to visits and diagnoses.
- Track portal and care coordination time when appropriate.
- Regularly review coding levels to avoid undercoding.
Small workflow changes can make a significant difference in both compliance and revenue.
How OptiMantra Supports Billing for Functional Medicine
Billing functional medicine is not just about choosing the right CPT codes. It’s about building a financial model that matches how your clinic actually delivers care.
Time-based coding allows clinics to bill appropriately for longer, more complex visits. Cash-pay models allow clinics to offer services that insurance may not cover. Hybrid models allow clinics to do both.
Billing functional medicine often involves a combination of insurance billing, time-based coding, memberships, packages, and cash-pay services. OptiMantra is designed to support these hybrid practice models by keeping clinical, scheduling, and financial workflows connected.
With OptiMantra, clinics can:
- Document total time for functional medicine visits within the EMR
- Support time-based E/M coding with appropriate documentation workflows
- Manage cash-pay services, memberships, and program packages
- Track visit utilization within membership plans
- Integrate scheduling with billing so visits link to charges correctly
- Maintain clear financial reporting across insurance and cash services
- Track lab orders and link them to diagnoses and visits
- Document care coordination and patient communication in the chart
- Reduce missed charges and undercoding through better workflow visibility
If your clinic feels like billing is more complicated than it should be, it’s usually a systems issue, not a coding issue. When documentation, scheduling, and billing are aligned, billing functional medicine becomes far more predictable and far more sustainable.
If you want to see how an integrated EHR and practice management system can support time-based coding, memberships, and hybrid billing models, you can explore OptiMantra with a personalized demo or start a free trial today!
Disclaimer: This content is for informational and educational purposes only and does not constitute legal, billing, or financial advice. Providers should consult qualified coding professionals, payers, and legal counsel to ensure compliance with current CPT®, payer, and state regulations when implementing time-based or cash-pay billing models.





.png)